Introduction
The incidence and prevalence of end-stage renal disease (ESRD) requiring renal replacement therapy (RRT) either by dialysis or kidney transplantation (KT) have progressively increased in countries around the world, including Korea [
1,
2]. Identifying ESRD incidence and prevalence is of vast importance so that policymakers and health care providers can develop public health care plans for ESRD patients. The Korean Society of Nephrology (KSN) launched a nationwide ESRD patient registry, Korean Renal Data System (KORDS), in 1985, which has continued for over 35 years. The goals of the KORDS are as follows: (1) to estimate the numbers and distributions of ESRD patients; (2) to determine the characteristics of ESRD and dialysis therapy and their complications or outcomes based on scientific evidence; and (3) to improve the quality of dialysis therapy and support public health decisions related to ESRD [
3]. Every year, the KSN releases an annual report from KORDS, which presents an overview of the incidence and prevalence of RRT including KT, the characteristics of patients, and the survival of patients on RRT in Korea. In this article, we provide a summary of the 2019 KORDS annual report. This article presents the most recent data on the epidemiology of RRT for ESRD, which focuses on the incidence and prevalence of RRT and ESRD mortality trends in Korea. More detailed data from the KORDS are available through the KSN website (
http://www.ksn.or.kr).
Methods
The KORDS was populated with responses from mailed paper questionnaires from 1985 to 1994. An electronic questionnaire with dial-up modem file transfer or diskette mailing was used from 1995 to 2000 [
4]. An internet-based questionnaire for dialysis patient registry has been administered by the KSN since 2001 via an online registry program on the KSN website and is updated yearly [
5]. Enrollment in the registry is voluntarily updated by members of the KSN. The registry program has collected data throughout the years, and the collected data include dialysis center information, dates of hemodialysis (HD) or peritoneal dialysis (PD) initiation, newly developed comorbid diseases, vascular access, dialysis doses, medications including erythropoiesis-stimulating agents and phosphorus-controlling agents, laboratory data, dialysis adequacy, rehabilitation status, and outcomes for each patient on HD, on PD, or who had undergone KT. Among these data, this study analyzed the changes in incidence and prevalence rates and outcomes in ESRD patients from 1986 to 2019. Because the survival data from 1986 to 2000 were insufficient, the analyses of incidence and prevalence of ESRD patients were performed from 1986 to 2019, but the analyses of outcomes were performed from 2001 to 2019. The KT recipients were excluded from outcome analysis. A flow diagram for patient selection is presented in
Supplementary Fig. 1 (available online). Trends in mortality rates are presented for the patients treated each year according to the number of patient-years at risk. Unadjusted survival rates were calculated using the Kaplan-Meier method, and absolute mortality rates were presented per 1,000 person-years of follow-up. All statistical analyses of survival data were analyzed using SAS (version 9.4; SAS Institute, Cary, NC, USA) and R (version 4.0.1; R Foundation for Statistical Computing, Vienna, Austria).
Discussion
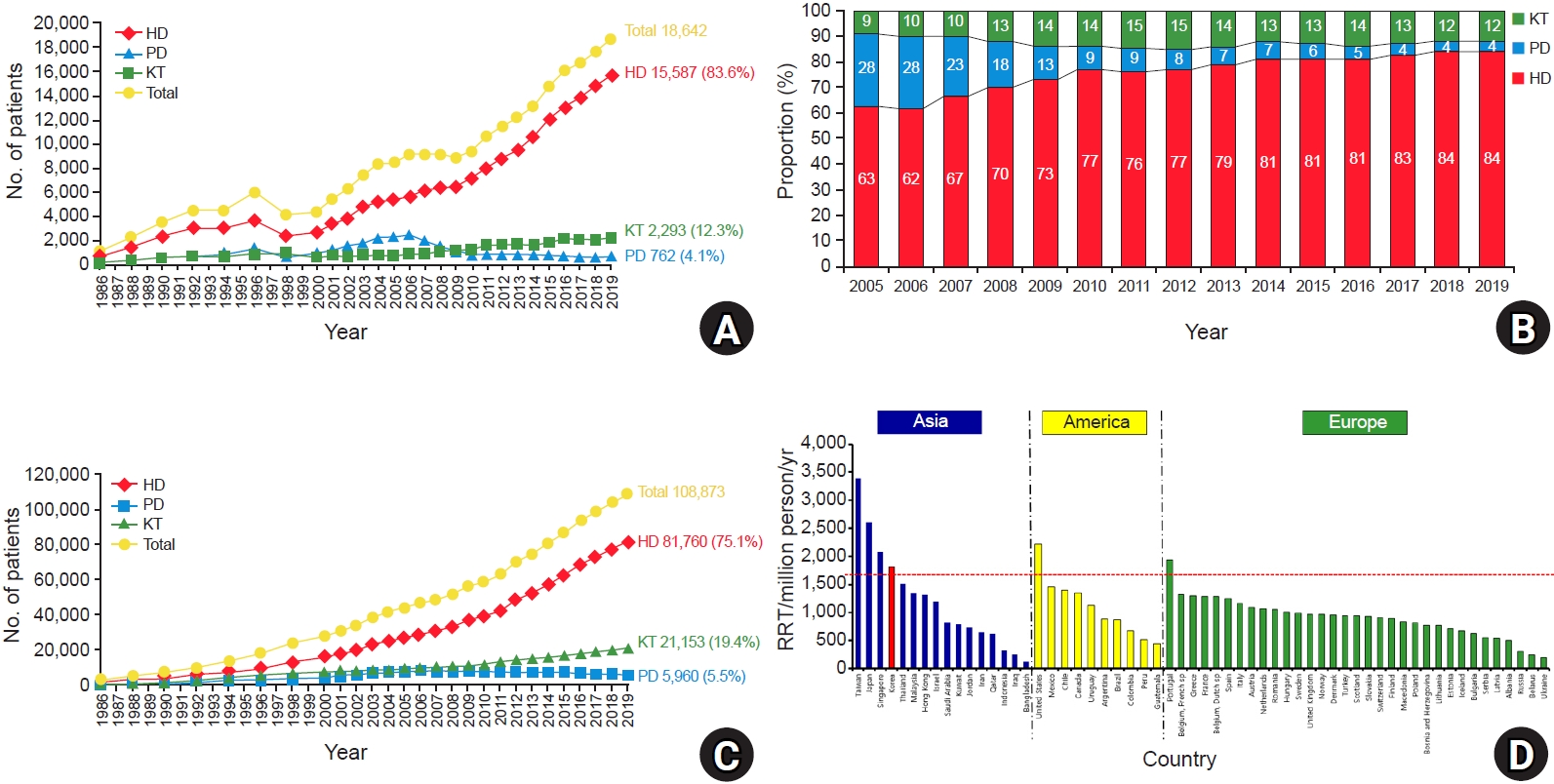
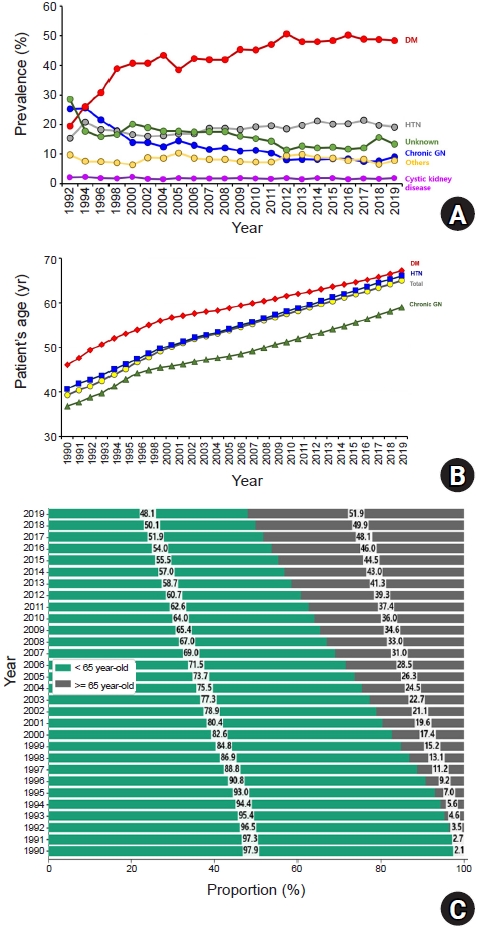
In the 2019 report of the KORDS, major findings included rapid growth in the overall number of patients undergoing dialysis, the proportion of elderly patients, and the overall number of patients undergoing long-term dialysis. The proportion of diabetic ESRD patients was maintained at around 50%, and a consistent decrease in the proportion of PD patients was observed in recent years. Among ESRD patients, the HD proportion in the study period increased to 84%, and the PD proportion decreased to 4%. Over the past two decades, the mortality of dialysis patients gradually decreased, but the mortality of diabetic dialysis patients was higher than that of dialysis patients with HTN or chronic GN. Recently, the patient survival rates in HD were similar to those in PD. Taken together, the survival improvement of dialysis patients and the increase in the proportion of long-term dialysis patients might contribute to the increase in the mean age of dialysis patients.
The incidence and prevalence of ESRD patients in Korea have been increasing over the past three decades, and the prevalence has doubled in the last 10 years. Although the prevalence of predialysis chronic kidney disease (CKD) stage 3 to 5 patients has remained constant during the same period [
8], the number of ESRD patients requiring RRT showed a recent rapid increase. As a result, Korea is now ranked sixth in the world for prevalence of ESRD [
9].
Although the data from KORDS in 2013 reported that the prevalence of ESRD patients did not appear to reach the inflection point [
10], the value has been continually increasing and has now exceeded those of Japan and the United States. At present, the trend resembles that of Taiwan, where the overall number of ESRD patients increased at the greatest rate among global countries [
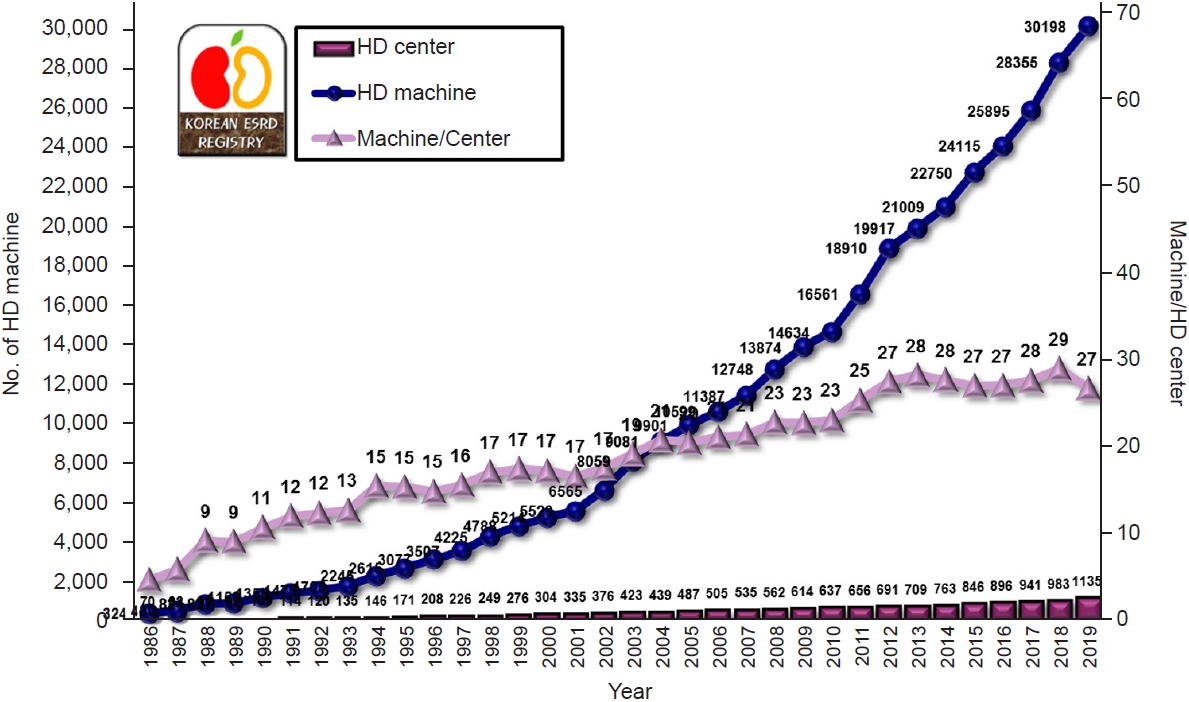
9]. The data from KORDS showed that most ESRD patients underwent HD. In the future, the aging trend will contribute to a progressively higher modality rate of HD compared to PD and KT. Under such circumstances, the numbers of HD centers and dialysis machines are likely to increase.
To reduce the number of ESRD patients, it is necessary to improve adherence through the proper administration of prescribed agents and lifestyle modifications according to the causative disease and to reduce complications through nephrologist counseling from the early stage of CKD. In addition, the rate of ESRD cases of unknown origin remains high, which must be resolved to reduce ESRD in the long term. Fortunately, regular health screenings via school, workplace, and regional systems have been expanded in Korea [
11]. Therefore, if a patient does not miss a regular health examination, data of unknown origin will gradually decrease through diagnosis of the causative disease.
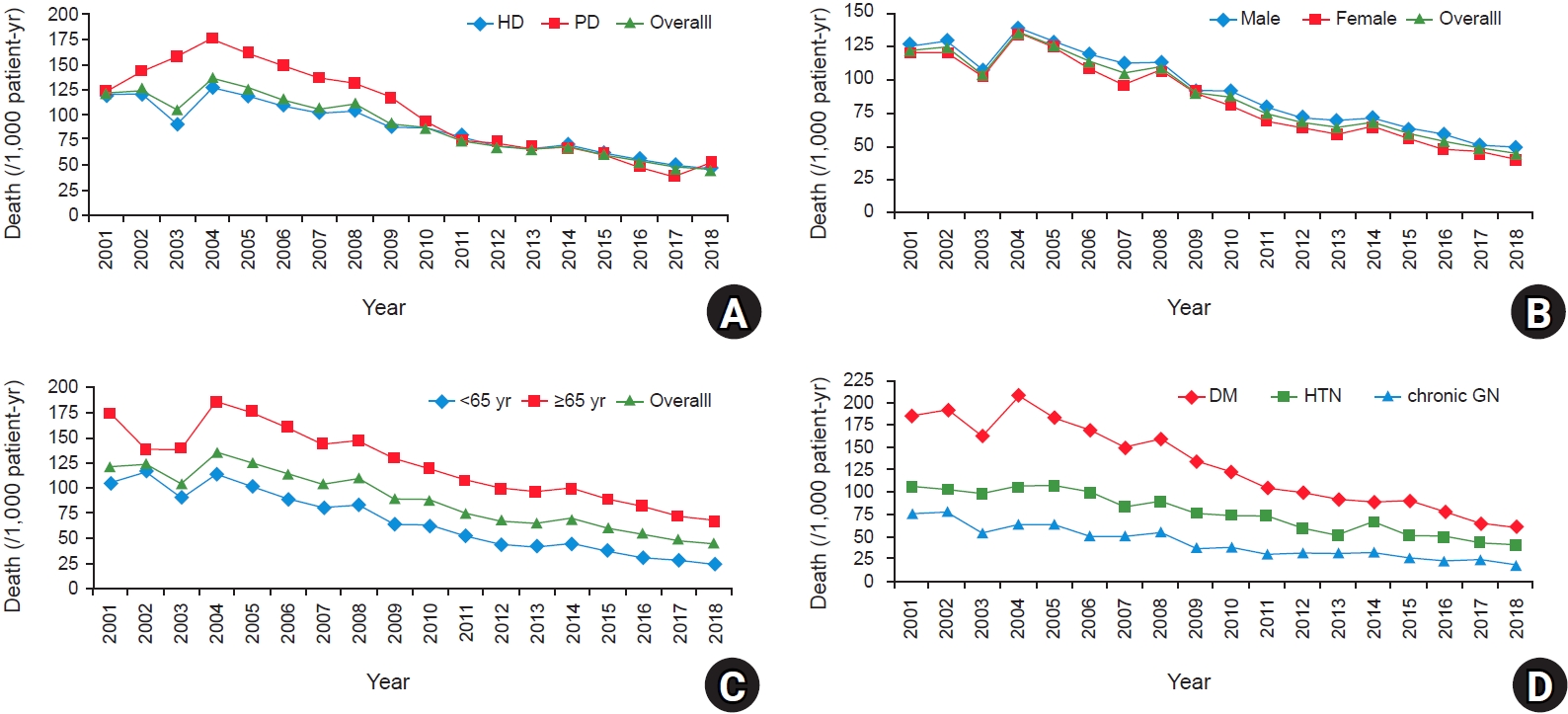
Another interesting finding was that the reduction in mortality risk was greater for patients treated with PD than those treated with HD in the past two decades, and that the survival of patients treated with PD and HD is similar in Korea for recent years. Comparisons between the long-term survival rates of patients with HD and PD in the past two decades were first reported in 2019 using the KORDS. In Korea, a previous population-based, large-scale study using Korean Health Insurance Review and Assessment data suggested that the mortality rate was significantly higher in incident PD patients than in incident HD patients in the period from 2005 to 2008 [
12]. On the other hand, PD was associated with better survival than HD in the early period of dialysis in a national prospective cohort study performed since 2009 [
13]. The present data from KORDS showed higher overall mortality rates in PD patients than in HD patients in the 2000s. Although the reason why PD patients have shown recent improvement in outcomes is not clear, it may be attributed to increased reimbursement for PD in the national health insurance program, the development of PD education programs, and the use of biocompatible PD solutions. Recent nationwide cohort data also indicated that PD and in-center HD provide similar survival in Europe and the United States [
1,
14]. Because statistical analyses for outcomes in this registry data were conducted without adjustment for confounding variables, further research is needed to assess the exact trends of mortality rates by treatment modality in Korean ESRD patients.
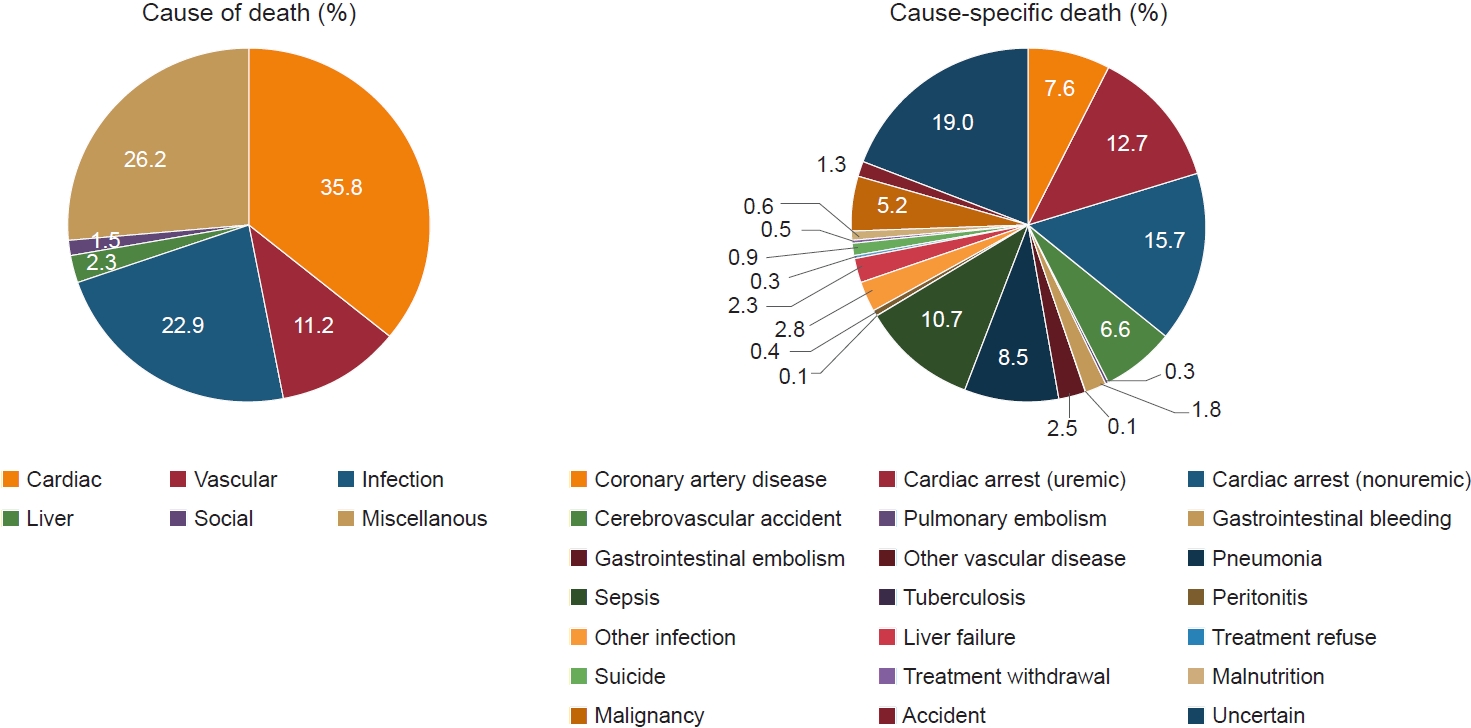
Despite a substantially decreasing trend of mortality rates in the last 20 years, the absolute mortality risk remains high in dialysis patients due to cardiovascular events and infections. In the KORDS for cause-specific death, cardiovascular disease was the most common, accounting for 47.0% of deaths (cardiac disease, 35.8% and vascular disease, 11.2%). Infection accounted for 22.9% of deaths and malignancy accounted for 5.0% of deaths in 2019. Trends in cause of death over time remained unchanged for cardiovascular disease and exhibited a mild increase for infection from 2001 to 2019. Other nationwide registry data demonstrated a decrease in cardiovascular mortality in dialysis patients over time in Japan and Europe [
6,
15]. However, survival analyses of the KORDS have some limitations, including relatively low enrollment rates, a lack of information on patient survival, and misclassification of cause-specific death, due to data collection based on voluntary enrollment. Therefore, it is necessary to consider a plan to increase the enrollment rate of the KORDS.
In conclusion, the KSN ESRD registry showed substantial increases in ESRD incidence and prevalence, especially in elderly and diabetic groups. These data highlight the need to pay attention to the high mortality rates of elderly and diabetic dialysis patients in Korea. These data also indicate the need for evidence-based treatment approaches for elderly and diabetic patients to prevent the progression of kidney disease. Although recent survival rates were similar between HD and PD patients, the proportion of prevalent PD patients gradually decreased. Therefore, further research may be needed for the individualized risk prediction of mortality regarding the selection of dialysis modality in patients who will start RRT.





















 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Supplement 1
Supplement 1 Print
Print















